Panel Series Session 3
Kiana Modavi, BA, and Teja Pattabhiraman, BA
June 2021
Executive Summary
On June 17th, 2021, Cal-IHEA and Connecting for Better Health convened a panel of experts for a discussion on data sharing to support whole person care efforts. The session highlighted the need for statewide Health Information Exchange (HIE) in California in order to gain a comprehensive view of the needs of individuals and to integrate different care services. By securely collecting and sharing data related to medical, behavioral health, and social services needs, we can improve care planning. Lisa Chan-Sawin (CEO, Transform Health), Beau Hennemann (Director of Special Programs, Anthem), and Diane Rittenhouse (Associate Professor, UCSF) joined moderator Timi Leslie (Founder and President, BluePath Health) to discuss how a robust HIE can critically improve care for vulnerable populations. The panel also discussed how to implement data-sharing with an eye for sustainability. This briefing is the final part of a three part series on HIE and Public Health, and is co-hosted by Cal-IHEA and the Connecting for Better Health Coalition. Watch the webinar recording here.
Lisa Chan-Sawin
Chan-Sawin kicked off the webinar by focusing on Alameda county’s successful Whole Person Care (WPC) pilot, where funding was used to implement data sharing procedures and platforms. Through building a full HIE incorporating both clinical and social data exchange, providers across different sectors were able to gain a comprehensive understanding of their patients’ challenges and psychosocial needs, which aided in crafting treatment plans. Further, Chan- Sawin called attention to how Alameda County leveraged its community-wide health records to serve the homeless population during the COVID-19 pandemic. Compared to other counties, Alameda was able to quickly identify and enroll eligible individuals into Medi-Cal through this new infrastructure.
Beau Hennemann
“At the end of the day, you can have the greatest piece of technology that’s available, but if you still have those legal barriers and that resistance to share the data, it doesn’t work. And Whole Person Care has really driven the needle forward there.”
Hennemann focused on the outcomes of the WPC pilots and how, despite the differences in system development, implementation and buy-in, counties are now in a stronger position to provide whole person care. Hennemann highlighted that even rudimentary data sharing infrastructure (e.g., some counties only established simple data feeds, meaning data still needed to be incorporated into a larger system) provided health plans with more information than they previously had access to, allowing better insight into services being provided by the county or community-based partners. Hennemann stressed that data exchange is a critical step to providing integrated care.
Diane Rittenhouse
Dr. Rittenhouse presented the data sharing toolkit her team developed as part of the Accountable Communities for Health Initiative, which aims to connect leaders across multiple sectors in addressing critical community health issues. The toolkit, developed based on key informant interviews and in-person site visits across the state, outlines and recommends data- sharing options for communities across the spectrum in terms of cross-sector data sharing.
From this qualitative research, seven parameters emerged, which serve as the framework for a community to assess their data-sharing maturity (along a continuum from beginner to advanced).
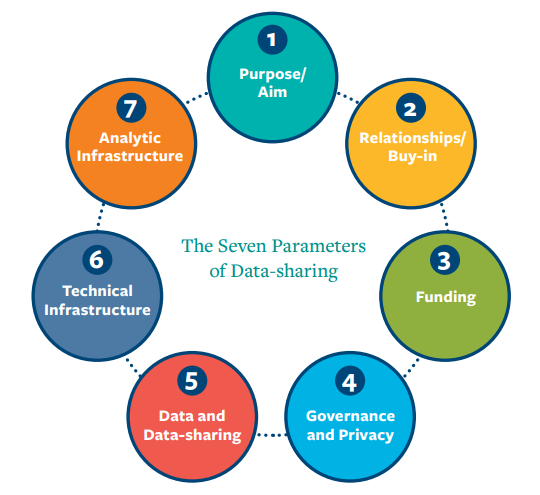
Dr. Rittenhouse discussed these seven shared parameters and how they play out in practice. She first emphasized the importance of having a clear purpose for data-sharing that is developed and agreed upon by all community stakeholders. This shared aim serves as the foundation for strong relationships between stakeholders and ensures that everyone has a seat at the table. She also discussed the importance of securing funding, whether through in-kind contributions, bond measures, state funding, or local foundations. These core elements—purpose, relationships, and funding— establish a foundation upon which communities are able to then progress along the parameters of governance, privacy, data elements, technical infrastructure, and analytic infrastructure. The process of developing a successful data-sharing system may move backwards, at times, to incorporate new strategies or involve new partners, and differs by community given differing priorities, perspectives, and funding sources. Dr. Rittenhouse emphasized that it is ultimately an iterative process, constantly evolving to meet the needs of a community.
Question and Answer
Timi (moderator): Lisa, where and how does universal consent happen at the community level, and what are the key pieces that need to happen all the way up to the state?
Lisa: Leveraging work done by the first-round pilot programs, we [in the Sacramento Whole Person Care pilot program] realized that we could structure our consent for the entire period of the program, meaning that we only needed to ask patients for their consent once. Having this universal consent tied back to the data-sharing agreement across all of our providers and partners meant that everybody was operating under the same rules and allowed the consent form to be available on the shared online care plan, so we didn’t have to ask the patient for the same consent multiple times.
It was also important to give everyone a seat at the table during the design of both the consent form and our data sharing agreement. We used a collective impact model and framework to bring everyone together so that we were operating in a transparent way.
Timi: Beau, how are you thinking about getting the data you need in order to continue supporting the work and track progress towards accomplishing the state’s goals?
Beau: As a health plan, we are engaging heavily with both counties and the state, and this is where the question around state versus county comes in. We can either use a county-by-county approach, or a statewide solution, which would be much more efficient and standardized. For example, a core component of CalAIM is addressing the needs of individuals who are transitioning out of the local jail and the state prison system and making sure they’re getting ongoing care coordination. Currently, there is a big disconnect in the data coming out of both the state prison and county jail system, and sometimes even between county probation and other county services. There is definitely room, from a statewide perspective, to break down these barriers, whether that be through a standardized data format or a centralized health information exchange system.
Timi: I want to unpack the challenge of participation. How do we get different organizations to participate in data sharing?
Beau: The big challenge, when it comes down to it, is that each organization interprets the rules differently. Even within one county, 10 organizations interpreting the rules differently makes it difficult to get buy-in to feed data into the system. Even after getting through the data sharing agreements, getting them to then commit to utilizing the system and embedding that into their day-to-day process is another challenge. It takes time, and the key is just being persistent and giving clear examples of how this is going to make care coordination better.
Timi: Diane, I was struck by the notion that data sharing actually builds trust. Can you give us a snapshot of what you learned when you looked at the community’s experience?
Diane: When we would ask communities how they share data, they would say “data only moves at the speed of trust”. It turned out that deep-rooted relationships, and the trust that is built within them, lead to the underlying buy-in that brings people to participate in the data-sharing efforts. Sometimes you want to start big, but a lot of these communities had really good experiences starting small, building trust, moving on to something a little bigger, bringing in more partners, having another success, and so forth; really just working that muscle of building trust.
Lisa: In Sacramento, we saw the same thing. We really couldn’t do the buildup we wanted to without trust. The standards of data sharing in healthcare are different than in housing. Clinical providers were initially concerned, expressing how the standards of data sharing in healthcare are different than in housing, and asking, can we really share data with housing providers in a seamless way? Their trust hadn’t been built yet. We had to take a step back and see what we could do to demonstrate that it could be done in a way that is protective of both the patients and the providers themselves. We’ve been able to demonstrate that there are ways to address the differences between privacy standards in clinical and social services, and also to think through how to build the systems and the flow of data in a way that is supportive of building that trust.
Timi: In addition to encouraging partnerships, it might be helpful to standardize assessments of trust. How might we start there, and is that something you’re seeing as a trend?
Beau: Standardization helps, to a certain extent. Each of the 29 counties is very different, and the needs of the people in each county are very different. We have to have some flexibility to account for these differences. But in terms of building trust and some additional standardization, it really does start with bringing people together, from the community-based organizations to the health plans and the community clinics– and putting the members at the center. You can’t have people coming it at with their own motives and what would be best for their organization– the question is, what will be best for the individual? How can we work together to make sure they get access to the services that they need?
Acknowledgements
Cal-IHEA thanks Connecting for Better Health for their leadership in organizing this panel event and for their partnership in writing the event proceedings.

